HPV and the Vaccine
What is HPV?
The human papillomavirus (HPV) is the most common sexually transmitted infection nationally and over 150 subtypes exist. In fact, most people who are sexually active will get infected at some point in their lives. HPV is spread through anal, vaginal, and oral sex, as well as intimate skin-to-skin touching.
What is the HPV vaccine?
The HPV vaccine prevents HPV infection protecting against the 9 types of HPV that most commonly cause HPV-related cancers. It has been available since 2006 with over 120 million doses of the HPV vaccine distributed since its FDA approval.¹
How safe/effective is the vaccine?
More than 12 years of research has shown that the HPV vaccination is safe, effective, and provides long-lasting protection against cancers caused by HPV infections.¹
Like any other vaccine, the HPV vaccine may cause mild side effects, such as redness or pain at the injection site, dizziness, or muscle pain. These are all temporary side effects and go away quickly.¹
Citation:
1. Centers for Disease Control and Prevention. (2020, November 16). HPV Vaccination is Safe and Effective. Retrieved from https://www.cdc.gov/hpv/parents/vaccinesafety.html.
What does HPV cause?
HPV is estimated to cause nearly 36,000 cases of cancer in men and women every year in the U.S.² Approximately 43% of men and women have genital HPV and about half of those are infected with high-risk types (22.7%). High-risk types are responsible for approximately 70% of HPV-associated cancer cases. In addition to cancers, HPV can also cause genital warts in all genders.
Cancer Statistics: Cancers caused by HPV ³
- 91% of cervical cancers
- 70% of throat cancers
- 90% of anal cancers
- 60% of cancers of the penis
- 75% of vaginal cancers
- 70% of cancers in the outside area of the vagina, called the vulva
HPV Health Disparities:
- Black and Hispanic women have higher rates of HPV-associated cervical cancer than women of other races and non-Hispanic women.⁴
- Hispanic women that live along the US-Mexico border currently have the highest incidence rates of cervical cancer.⁵
- It is estimated that about 1,300 new cases of HPV-associated cancers of the penis are diagnosed in the United States each year. Hispanic men have higher rates of HPV-associated penile cancer than non-Hispanic men.⁴
Citations:
2. Centers for Disease Control and Prevention. (2020, November 19). About HPV. Retrieved from https://www.cdc.gov/hpv/parents/about-hpv.html.
3. National Cancer Institute. (2020, November 18). HPV and Cancer. Retrieved from https://www.cancer.gov/about-cancer/causes-prevention/risk/infectious-agents/hpv-and-cancer#cancers-caused.
4. Centers for Disease Control and Prevention. (2020, November 18). HPV-Associated Cancer Rates by Race and Ethnicity. Retrieved from https://www.cdc.gov/cancer/hpv/statistics/race.htm.
5. Mann, L., Foley, K. L., Tanner, A. E., Sun, C. J., & Rhodes, S. D. (2015). Increasing cervical cancer screening among US Hispanics/Latinas: A qualitative systematic review. Journal of Cancer Education, 30(2), 374-387.
How many shots are needed?
The HPV vaccine is recommended for all genders ages 9 to 26 years old. Some adults 27 to 45 years old who have not completed the HPV vaccine series may get the vaccine based on a discussion with their health care provider. Depending on age, the schedule will require either 2 or 3 vaccines.
A 2-dose schedule is recommended for people who get the first dose before their 15th birthday. In a 2-dose series, the second dose should be given 6–12 months after the first dose (0, 6–12 month schedule).⁶

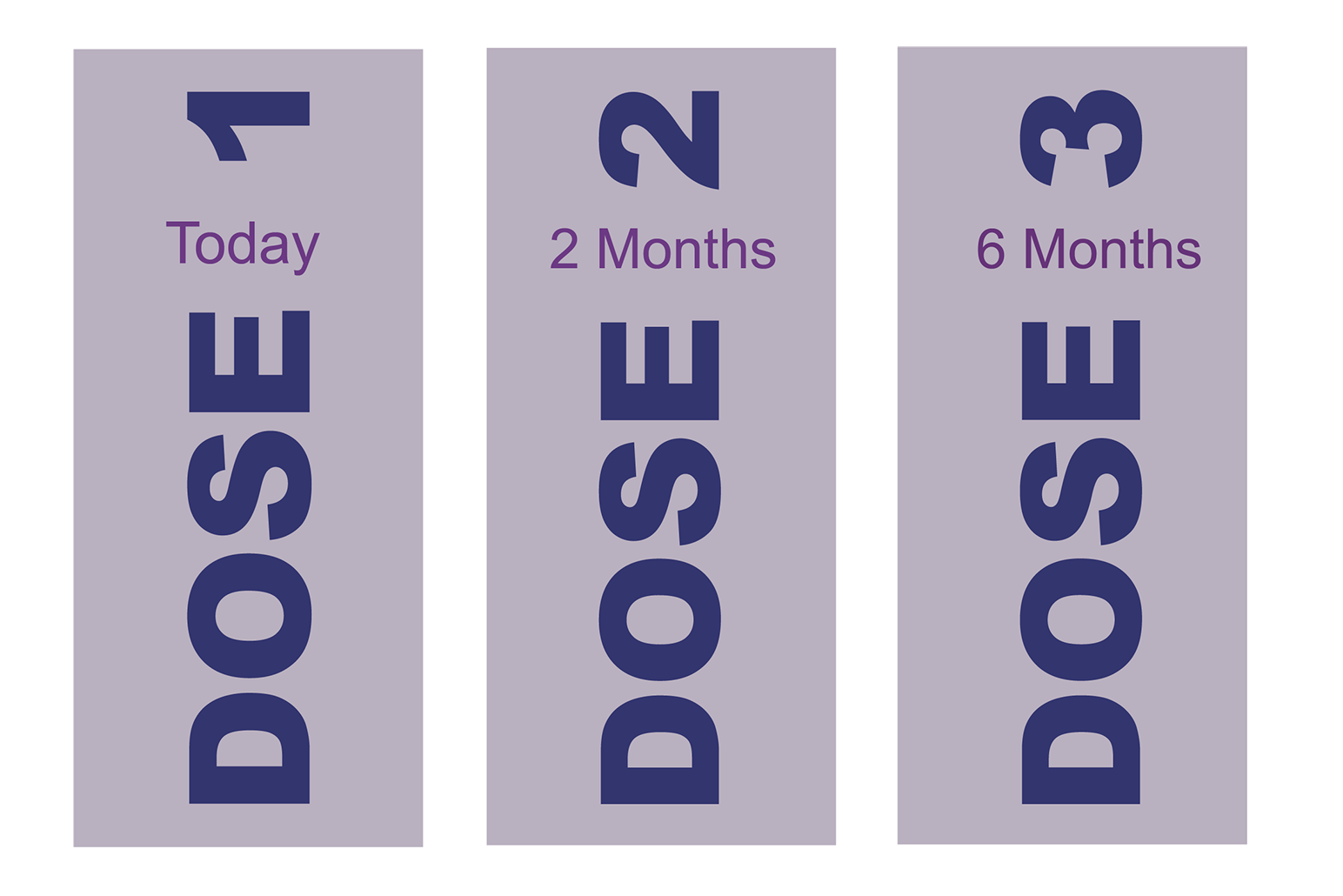
A 3-dose schedule is recommended for people who get the first dose on or after their 15th birthday, and for people with certain immunocompromising conditions. In a 3-dose series, the second dose should be given 1–2 months after the first dose, and the third dose should be given 6 months after the first dose (0, 1–2, 6-month schedule).⁶
Citation:
6. Centers for Disease Control and Prevention. (2020, November 16). HPV Vaccine Schedule and Dosing. Retrieved from https://www.cdc.gov/hpv/hcp/schedules-recommendations.html.
